Tackling Traction
Cleat Design Matters
Research shows that cleat design directly influences how much grip an athlete experiences. When there is too much rotational traction, the foot can “lock” to the surface, driving torque up the leg and into the knee.
Key Takeaway: Cleats are part of the injury risk equation.
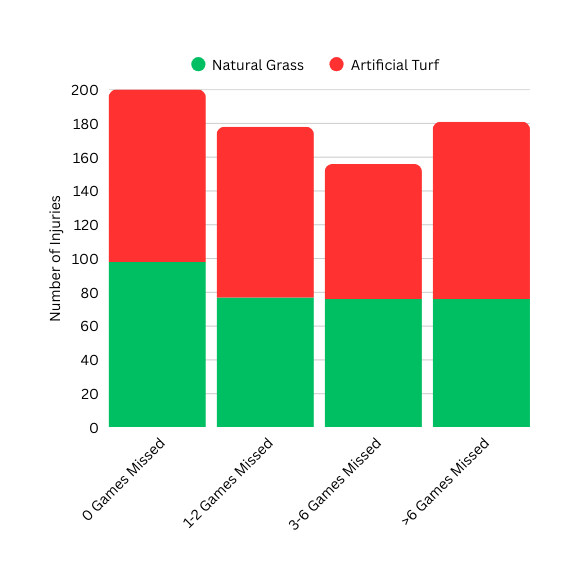
Surface Conditions Influence Traction
NFL Epidemiology (2021-2022) showed higher rates of lower-extremity injuries on turf versus natural grass. Artificial surfaces deliver higher rotational stiffness, sometimes exceeding thresholds linked to injury risk.
Key Takeaway: The surface is notorious for its contribution to injury risk.
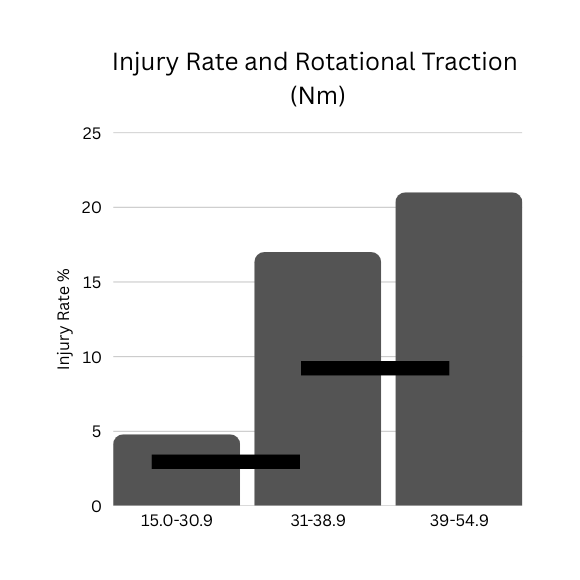
Traction & Injury: The Connection
Biomechanical reviews link higher rotational resistance at the shoe–surface interface with increased risk of ACL and other lower-extremity injuries. It’s not ONLY “turf vs. grass,” but whether the rotational torque exceeds safe levels.
Key Takeaway: Non-contact lower-extremity injuries are strongly tied to excessive rotational traction - a result of current surface and footwear design.

How Caddix Solves the Traction Problem
Our SmartStuds™ flex and release under load. Instead of locking the foot in place, SmartStuds™ deform slightly during pivoting and cutting, allowing for quicker stud release from the playing surface. This reduces rotational torque on the knees and ankles without sacrificing the traction athletes need for acceleration and cutting.
By targeting safe rotational stiffness ranges identified in biomechanical research, Caddix cleats strike the balance between performance and protection.
Unlike traditional rigid studs, SmartStuds™ adapt to both turf and grass, moderating rotational resistance across surfaces where injury risks typically rise.
Nothing can prevent injury, but Caddix SmartStuds™ take a leap toward risk mitigation.
-

A company is developing cleats for women soccer players to decrease knee injuries
Listen here -

Pat McAfee & Joe Flacco talk about Caddix Cleats on Pat's show (11:50 in)
Watch here -

Former football player reducing injury in sport with invention
Read here -

A great 5-minute segment about the idea and the visionaries behind it.
Watch now -

Dennis Pitta and Todd Heap invest in cleat company Caddix
Read here -

Former Ravens Todd Heap, Dennis Pitta invest in Caddix Cleats
Read here -

2 former Ravens hope this cleat company can change football
Read here -

Caddix Cleats adds Todd Heap, Dennis Pitta as majority investors
Read here -

Portland's i-Generator works with Nike, Adidas, and startups
Read here -

Joe Flacco debuted new cleats that could change the NFL forever
Read here -

This New Cleat is Designed to Prevent Knee Injuries
Read here










